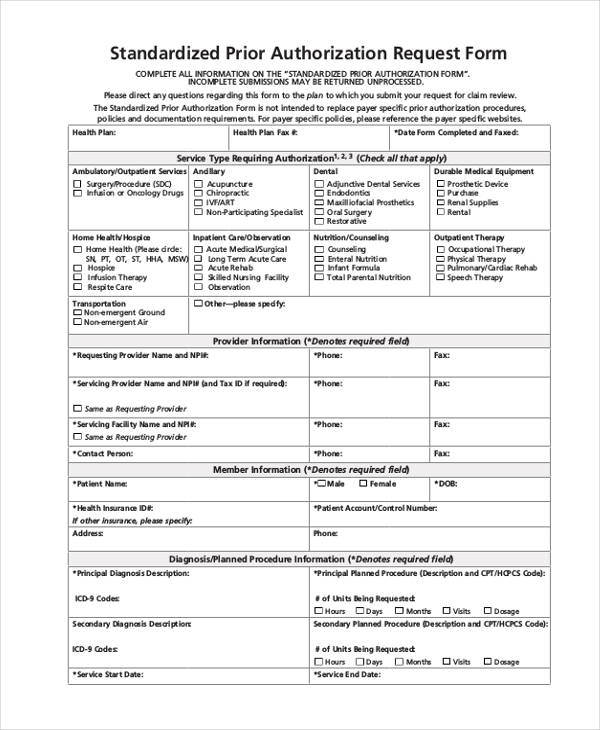
Standard Prior Authorization Form
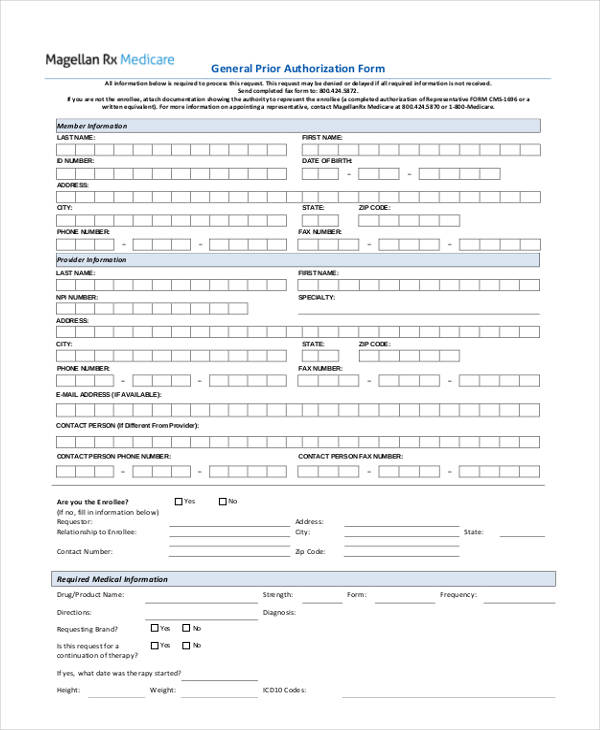
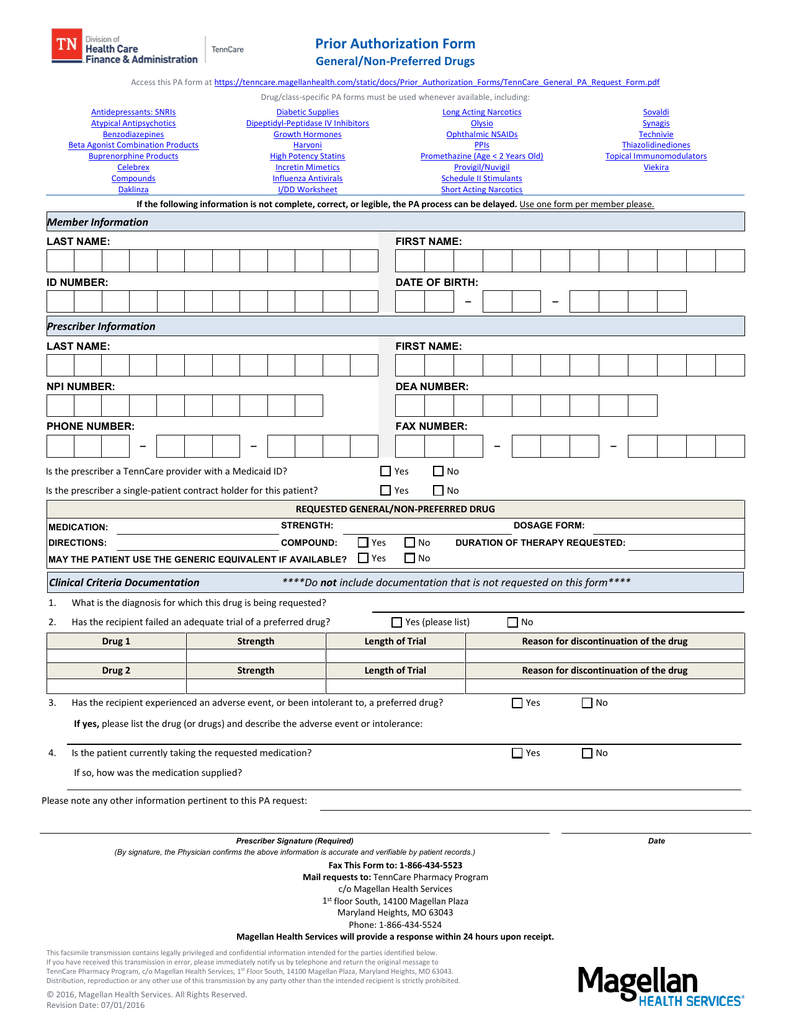
Standard Prior Authorization Form - Web what is the purpose of the form? ☐ initial request continuation/renewal request reason for request (check all that apply): It is intended to assist providers by streamlining the data submission process for selected services that. Web massachusetts standard form for medication prior authorization requests *some plans might not accept this form for medicare or medicaid requests. An attestation was added as a certification that any request submitted with the expedited timeframe meets the cms criteria. 4) request a guarantee of payment; Web standardized prior authorization request form standardized prior authorization request form 3 this form does not replace payer specific prior authorization requirements. Requesting providers should attach all pertinent medical documentation to support the request and submit to cca for review. This form is being used for: Web ohio department of medicaid | 50 west town street, suite 400, columbus, ohio 43215.
Do not use this form to: Web electronically, through the issuer’s portal, to request prior authorization of a health care service. The form is designed to serve as a standardized prior authorization form accepted by multiple health plans. Web what is the purpose of the form? The prior authorization request form is for use with the following service types: Web standardized prior authorization request form standardized prior authorization request form 3 this form does not replace payer specific prior authorization requirements. Web cca has a new standardized prior authorization form to ensure that minimal processing information is captured. Web ohio department of medicaid | 50 west town street, suite 400, columbus, ohio 43215. Web massachusetts standard form for medication prior authorization requests *some plans might not accept this form for medicare or medicaid requests. ☐ initial request continuation/renewal request reason for request (check all that apply):
This form is being used for: Web cca has a new standardized prior authorization form to ensure that minimal processing information is captured. Web the standardized prior authorization form is intended to be used to submit prior authorization requests by fax. Web standardized prior authorization request form standardized prior authorization request form 3 this form does not replace payer specific prior authorization requirements. It is intended to assist providers by streamlining the data submission process for selected services that. The prior authorization request form is for use with the following service types: ☐ prior authorization, step therapy, formulary exception Requesting providers should attach all pertinent medical documentation to support the request and submit to cca for review. An attestation was added as a certification that any request submitted with the expedited timeframe meets the cms criteria. Web electronically, through the issuer’s portal, to request prior authorization of a health care service.
FREE 13+ Prior Authorization Forms in PDF MS Word
☐ initial request continuation/renewal request reason for request (check all that apply): An attestation was added as a certification that any request submitted with the expedited timeframe meets the cms criteria. Do not use this form to: 4) request a guarantee of payment; The prior authorization request form is for use with the following service types:
Fillable Texas Standard Prior Authorization Request Form For Health
An attestation was added as a certification that any request submitted with the expedited timeframe meets the cms criteria. The form is designed to serve as a standardized prior authorization form accepted by multiple health plans. Web the standardized prior authorization form is intended to be used to submit prior authorization requests by fax. This form is being used for:.
20152022 AL BCBS Form ENR469 Fill Online, Printable, Fillable, Blank
This form is being used for: Requesting providers should attach all pertinent medical documentation to support the request and submit to cca for review. The prior authorization request form is for use with the following service types: Web what is the purpose of the form? Web cca has a new standardized prior authorization form to ensure that minimal processing information.
FREE 13+ Prior Authorization Forms in PDF MS Word
4) request a guarantee of payment; An attestation was added as a certification that any request submitted with the expedited timeframe meets the cms criteria. ☐ prior authorization, step therapy, formulary exception The prior authorization request form is for use with the following service types: This form is being used for:
Fillable Texas Standard Prior Authorization Request Form For Health
The new form is now available for download on the cca website. Web the standardized prior authorization form is intended to be used to submit prior authorization requests by fax. The prior authorization request form is for use with the following service types: Web standardized prior authorization request form standardized prior authorization request form 3 this form does not replace.
Prior Authorization Form
Web electronically, through the issuer’s portal, to request prior authorization of a health care service. Web massachusetts standard form for medication prior authorization requests *some plans might not accept this form for medicare or medicaid requests. The form is designed to serve as a standardized prior authorization form accepted by multiple health plans. An attestation was added as a certification.
Fillable Therapy & Home Health Prior Authorization Standard Request
Web electronically, through the issuer’s portal, to request prior authorization of a health care service. Web standardized prior authorization request form standardized prior authorization request form 3 this form does not replace payer specific prior authorization requirements. Web what is the purpose of the form? Do not use this form to: It is intended to assist providers by streamlining the.
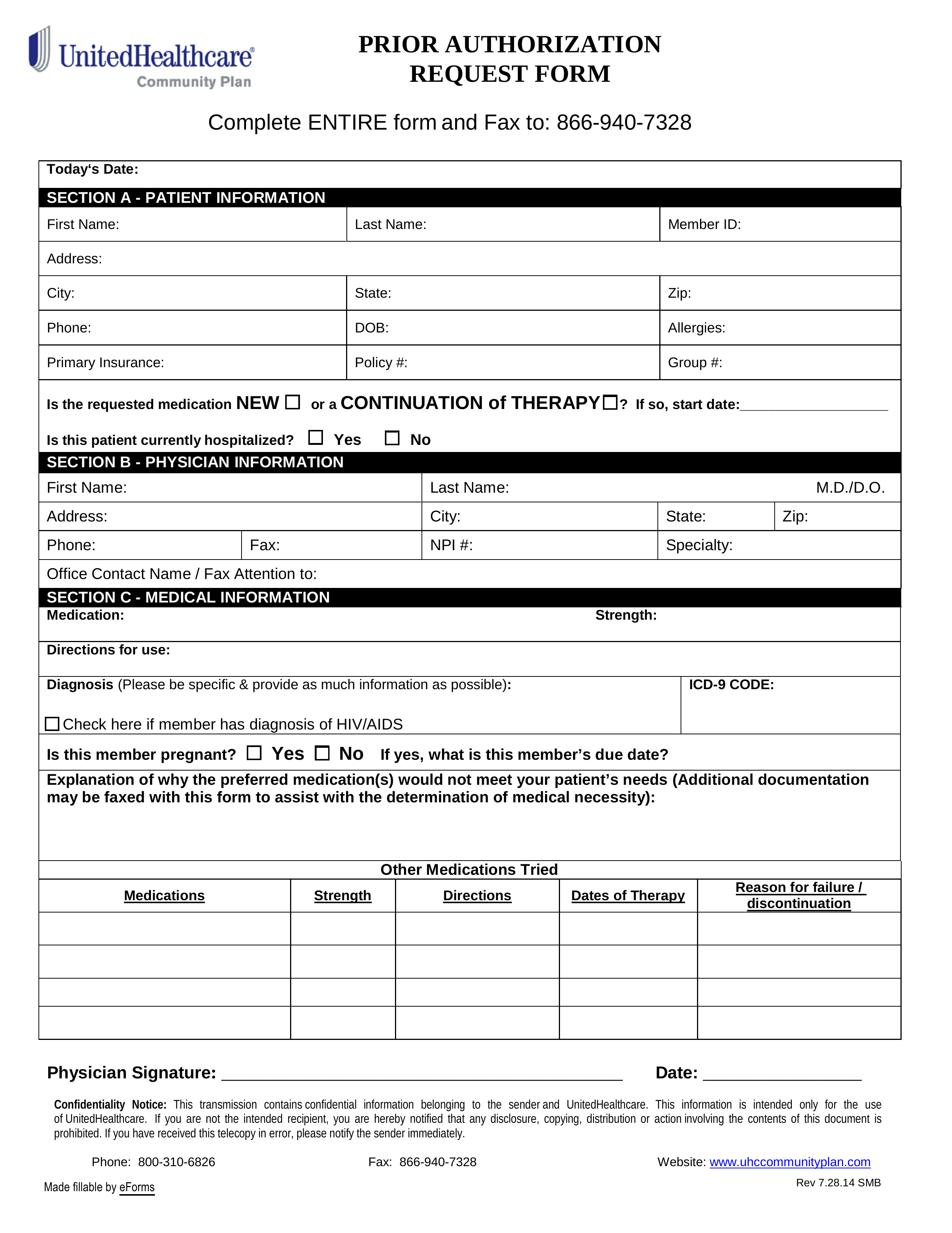
Free UnitedHealthcare Prior (Rx) Authorization Form PDF eForms
Web ohio department of medicaid | 50 west town street, suite 400, columbus, ohio 43215. Web electronically, through the issuer’s portal, to request prior authorization of a health care service. Do not use this form to: The new form is now available for download on the cca website. It is intended to assist providers by streamlining the data submission process.
FREE 13+ Prior Authorization Forms in PDF MS Word
The prior authorization request form is for use with the following service types: It is intended to assist providers by streamlining the data submission process for selected services that. ☐ prior authorization, step therapy, formulary exception 4) request a guarantee of payment; Do not use this form to:
Fillable Prior Authorization Standard Request Form printable pdf download
Requesting providers should attach all pertinent medical documentation to support the request and submit to cca for review. The prior authorization request form is for use with the following service types: Do not use this form to: Web what is the purpose of the form? Web the standardized prior authorization form is intended to be used to submit prior authorization.
☐ Prior Authorization, Step Therapy, Formulary Exception
Web electronically, through the issuer’s portal, to request prior authorization of a health care service. Web cca has a new standardized prior authorization form to ensure that minimal processing information is captured. The new form is now available for download on the cca website. Web what is the purpose of the form?
4) Request A Guarantee Of Payment;
The prior authorization request form is for use with the following service types: Requesting providers should attach all pertinent medical documentation to support the request and submit to cca for review. The form is designed to serve as a standardized prior authorization form accepted by multiple health plans. ☐ initial request continuation/renewal request reason for request (check all that apply):
Web Standardized Prior Authorization Request Form Standardized Prior Authorization Request Form 3 This Form Does Not Replace Payer Specific Prior Authorization Requirements.
Do not use this form to: Web the standardized prior authorization form is intended to be used to submit prior authorization requests by fax. An attestation was added as a certification that any request submitted with the expedited timeframe meets the cms criteria. Web massachusetts standard form for medication prior authorization requests *some plans might not accept this form for medicare or medicaid requests.
Web Ohio Department Of Medicaid | 50 West Town Street, Suite 400, Columbus, Ohio 43215.
This form is being used for: It is intended to assist providers by streamlining the data submission process for selected services that.